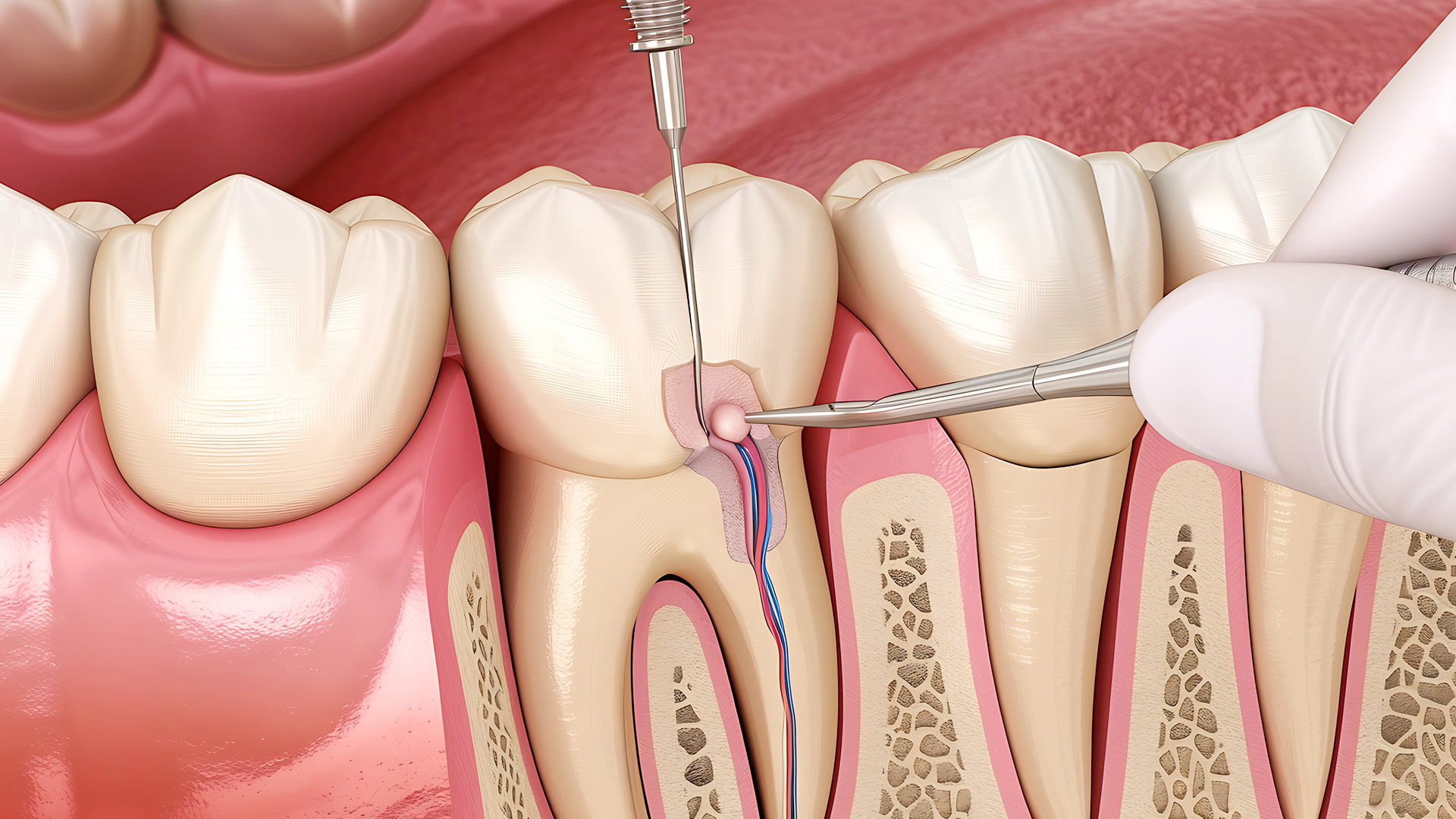
“Root canal” Those two words have been sufficient to put perfectly reasonable adults into a cold sweat for years. However, recently, your colleague, friend, or relative may tell you that he or she has one, and even say, I did not feel anything. What changed? Has dentistry all at once acquired magic powers? In this article, we’ll explore the real science pushing a new generation of virtually painless root canal treatments. We will consider the anaesthesia of today, smarter equipment, anti-infection technology, and even the psychology behind the comfort in the dental chair.
Redefining Pain: The Anaesthetic of the Present Day
The fear of needles or numb lips may keep others from going to the dentist, yet local anaesthesia has undergone its own makeover.
The Chemistry of Comfort
- Newer agents of anaesthesia, articaine and mepivacaine, have been shown to diffuse through bone more effectively than older lidocaine formulas.
- The buffered anaesthetic is made to match the normal pH of the body, which makes it less painful to inject, and it takes about half the time to work.
- The computer-controlled delivery systems, like The Wand, discharge the anaesthetic in a constant and low pressure that patients tend to interpret as pressure instead of pain.
“Numbness isn’t the goal, comfort is,” notes Dr Sonia Gupta, an endodontist in Chicago. “When patients don’t feel the shot going in, they finally believe us when we say the root canal itself won’t hurt.”
Supplemental Intraosseous and PDL Injections
Dentists can also avoid the normal nerve pathways; even when a tooth is hot (inflamed and difficult to numb), it is possible to bypass the nerve.
- Intraosseous injection: A tiny hole is drilled into the bone adjacent to the tooth; an anaesthetic is injected directly into the nerve bundle.
- Periodontal ligament (PDL) injection: This is a thin needle that injects the ligament space and only anaesthetises the tooth itself- excellent when you must speak after it.
Such improvements come with complete numbness in one to two minutes, as compared to the conventional 10-15.
Rotary, Reciprocating, and Gentle Wave: Tissue-Saving tools.
Dentists in the 1990s used to hand-file canals with stainless-steel files for half of the appointment. It was not only slow but it produced friction and heat, which irritated tissues.
Nickel-Titanium Rotary Files
- Able to bend around sharp curves along canals without transport (cutting the wrong path).
- They are super-elastic and require fewer files to be inserted, saving chair time.
- The rotating motion is smooth and removes the infected dentin, producing fewer cracks in the root.
Reciprocating Systems
These files do not rotate continuously, but move back and forth in a fixed arc:
- Less torsional stress = lower chance of instrument separation.
- Short pecking motions imply light contact, which translates to less postoperative pain.
Ultrasonic & Multi Sonic Irrigation (Gentle Wave)
Gentle Wave is a multi-sonic fluid-based system that employs microscopic files that are flushed using tiny acoustic waves and broad-range frequencies to remove bacteria and debris from microscopic canal branches that most files fail to reach. Less dentin is removed, resulting in the tooth remaining stronger.
According to a peer-reviewed article published in the Journal of Endodontics in 2016, multi sonic irrigation can remove up to 97% of biofilm in lateral canals, where conventional methods can only remove 60 – 70%.
Lasers, Ozone, and Photodynamic Therapy: Beyond Bleach.
Conventional root canals use sodium hypochlorite, or more often referred to as bleach, which is used to disinfect. Although successful, chemical irrigation may fail to remove viable bacteria in complex anatomy.
Laser-Assisted Endodontics
Er: YAG and Nd: YAG lasers release energy, which vaporises any tissue residues and bacterial walls:
- Photon-induced photoacoustic streaming (PIPS): micro-bubbles form and burst against the canal walls due to the pulse of a laser tip inserted in the pulp chamber (not the canal) and direct the energy through the irrigant.
- It has benefits such as less instrumentation, less smear layer, and lower scores on postoperative pain in clinical trials.
Ozone Gas and Photodynamic Therapy (PDT)
- Ozone (O 3) is an effective oxidiser that destroys bacteria, viruses, and fungi in a few seconds and decomposes to oxygen, leaving no remains
- PDT combines a light of a particular wavelength with a photosensitizer dye to produce reactive oxygen species that are deadly to microorganisms.
Neither is a replacement for traditional irrigation, although perhaps more of a complement, but both techniques serve to understand why most patients mention that they feel less sore after the treatment- there is less leftover infection.
3D Imaging, AI Planning: See It, Then Treat It.
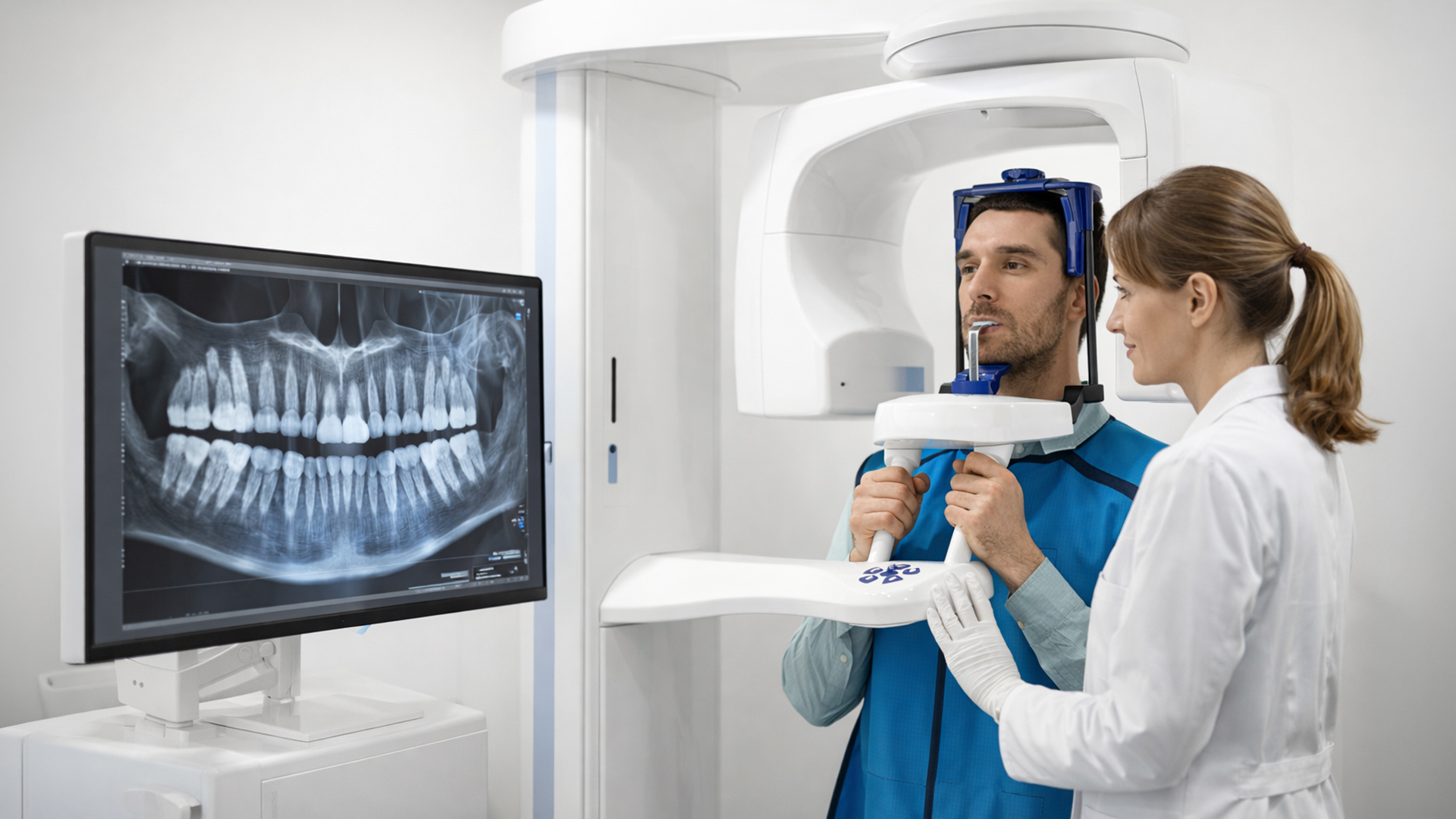
Cone Beam Computed Tomography (CBCT)
CBCT records a 3-D map of the tooth and bone in the vicinity:
- Finds additional canals that have the potential to be infected in case they are missed.
- Exposes fractures or resorptive defects to enable the dentist to forecast success or propose alternatives.
Artificial-Intelligence Diagnostics
The programme, like Endo Vision AI, can scan CBCT data and identify possible canals and periapical lesions to enable clinicians to plan with precision. The fewer guesses made, the fewer surprises, the shorter the appointment, and, in the end, the less physical stress on the patient.
It was like watching a small planet being explored as I saw a 3-D image of my molar on the screen. Suddenly, it all appeared to make sense, not frightening, a personal reflection on the personal experience of the author of the same treatment last year.
Psychology & The Pain Paradox
Pain perception is partially in the head, regardless of the state-of-the-art tools.
The Cortisol Connection
Dental anxiety increases cortisol, the stress hormone of the body, and may increase pain sensitivity. Contemporary practices address this with:
- Noise-cancellation headphones and ceiling TVs.
- Mindfulness or short breathing in the operatory.
- Effective communication-seeing the process helps to eliminate uncertainties, which is the root cause of most fear.
Local anaesthetic with Nitrous = A Stress-Free Brain
Inhaled nitrous oxide (laughing gas) does not leave you unconscious, but it dulls the fear response of the amygdala. The two-pronged strategy maintains a lower heart rate and cortisol, and the anaesthetic labour more efficiently. Reduced biologic stress can be translated to faster healing.
Future: Bio-ceramic Sealers and Regenerative Endodontics
Bio-ceramic Sealers
Conventional gutta-percha fillings are now used in combination with calcium-silicate-based sealers, which:
- Elaborate a little on the setting, filling microscopic gaps.
- Be above PH 12, unfriendly to leftover bacteria.
This is beneficial to the patients since the relapse rate reduces significantly with a tighter seal, one of the reasons that the older generation was afraid that they might experience lingering pain following a root canal.
Regenerative Procedures
Clinicians can induce the growth of pulp-like tissue on the root of immature teeth, so the root can complete its development- no fillers necessary. Although it is still a niche, there is an indication of a day when the term, root canal, will be replaced with the word, pulp revitalisation.
Conclusion
Advanced disinfection, smarter instruments, modern anaesthesia, more accurate imaging, and a more accurate comprehension of patient psychology have all come together to make root canal therapy a more or less comfortable routine. Whenever someone tells you that they had a painless root canal, they are telling the truth; it is not hyperbole in the marketing sense of the term, but it is science doing its mute business.
And in case you have been putting off seeing the dentist about that sore molar, then you may want to make an appointment. An hour-long visit today at Premiere Dental would save you hours of pain tomorrow, and you would be glad to see how you would feel in the chair.