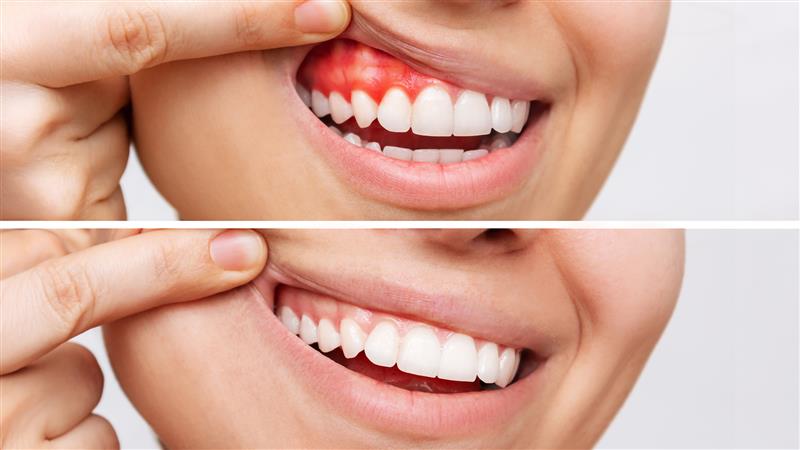
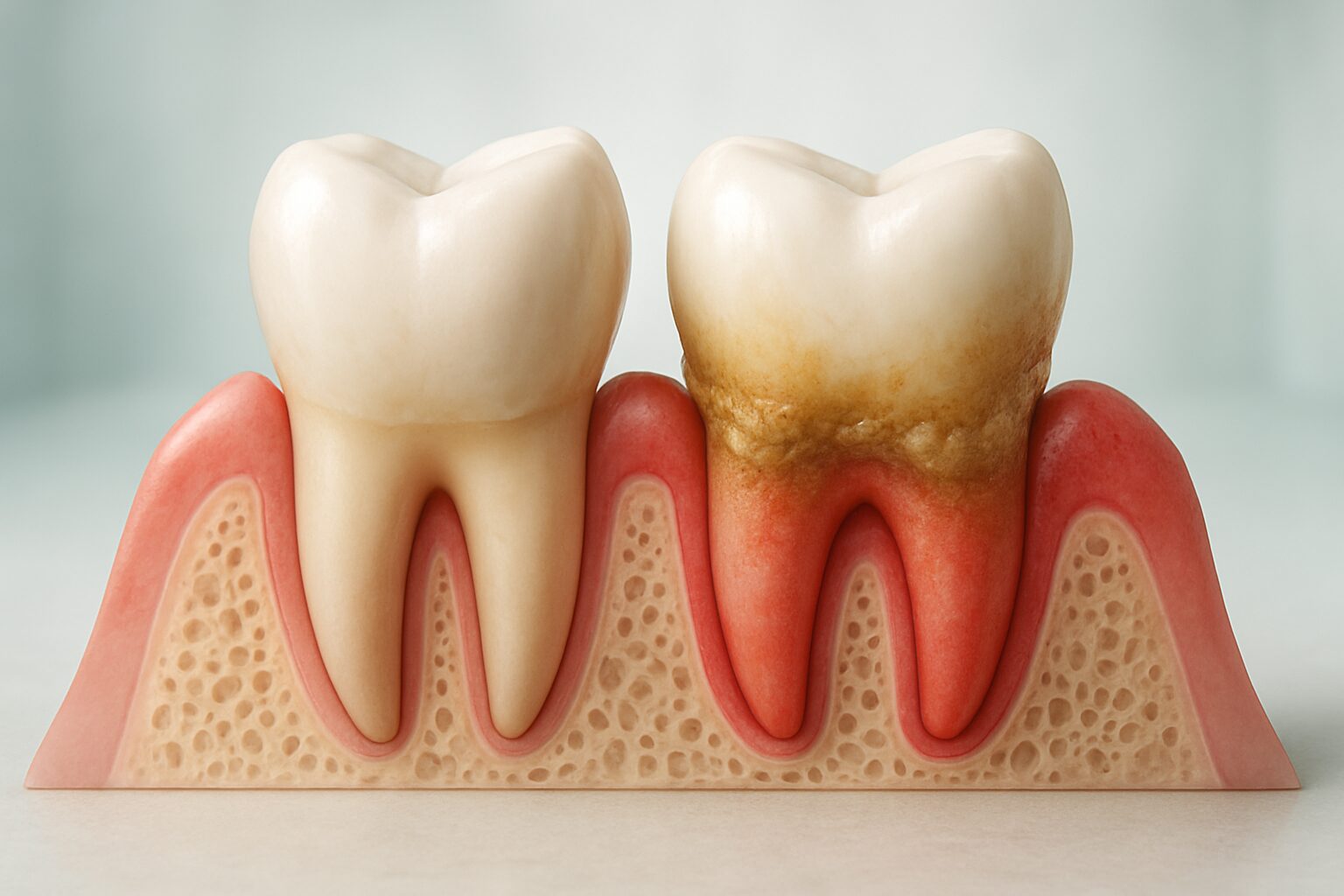
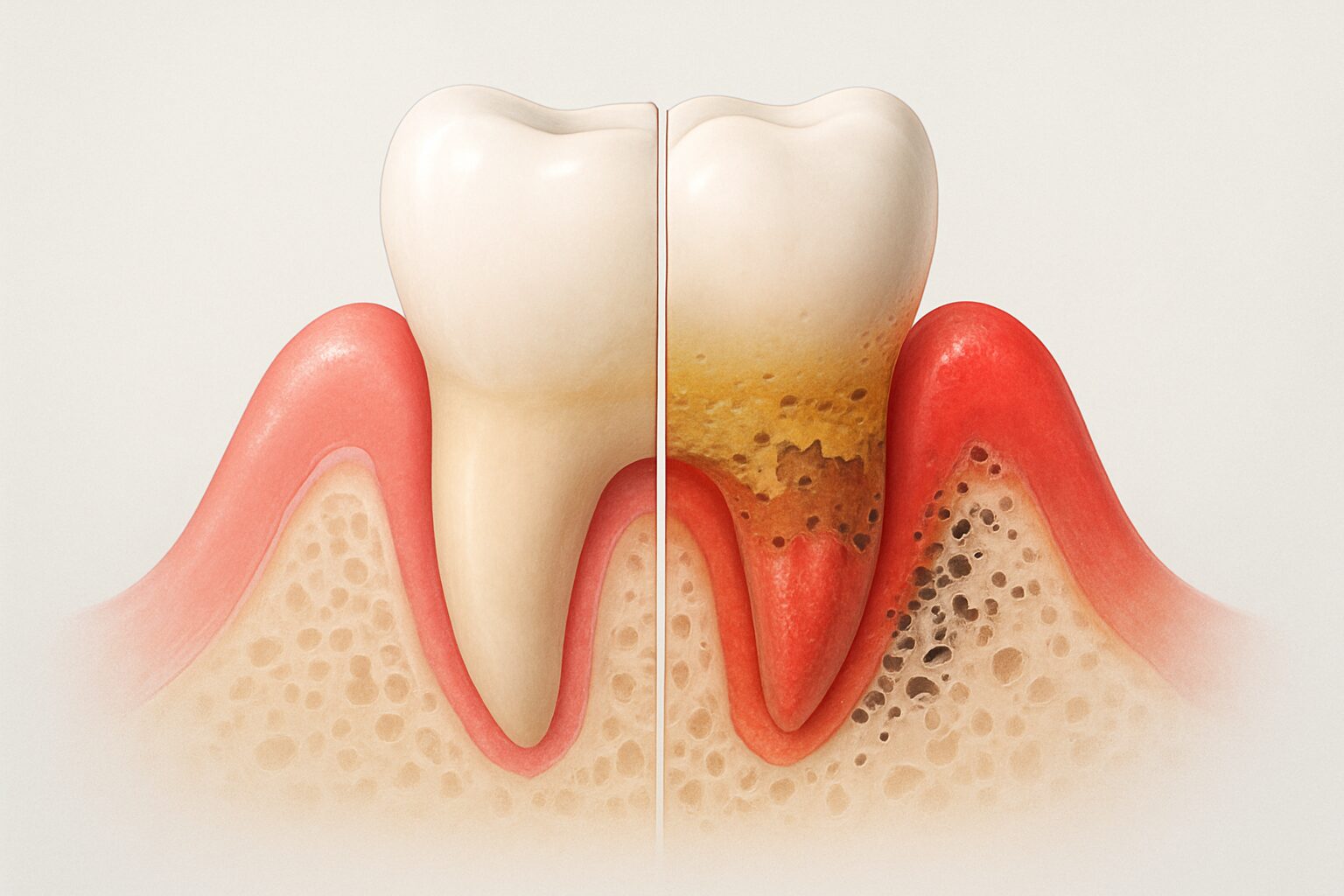
Gum disease starts as mild inflammation but can progress to tooth loss and serious health complications when left untreated. Early detection and proper prevention make all the difference in maintaining healthy gums for life.
This article examines the underlying causes that contribute to the development of gum disease, ranging from poor oral hygiene to genetic factors. Readers will discover proven daily habits that promote gum health, including specific brushing techniques and dietary recommendations. The guide also covers professional treatments available to reverse existing gum damage and lifestyle changes that strengthen natural gum defenses against harmful bacteria.
Understanding Gum Disease and Its Impact on Your Health
What Gum Disease Really Is and Why It Matters
Gum disease represents a bacterial infection that targets the tissues surrounding and supporting teeth. This condition begins when harmful bacteria accumulate along the gumline, forming a sticky film called plaque. When plaque remains undisturbed, it hardens into tartar, creating an ideal environment for bacteria to thrive and multiply.
The condition affects millions of people worldwide, making it one of the most prevalent oral health issues. Despite its common occurrence, many people underestimate the serious implications of untreated gum disease. The infection doesn’t limit itself to the mouth – research consistently demonstrates strong connections between gum disease and various systemic health conditions, including heart disease, diabetes, and respiratory infections.
Professional dental organizations classify gum disease into two primary stages: gingivitis and periodontitis. Gingivitis represents the milder, reversible form, while periodontitis involves more severe tissue damage that can become irreversible without proper intervention.
Early Warning Signs You Should Never Ignore
Recognizing the initial symptoms of gum disease enables early intervention and prevents progression to more serious stages. The earliest indicators often appear subtle, which explains why many people overlook them until the condition advances.
Physical Symptoms:
-
Red, swollen, or tender gums
-
Bleeding during brushing or flossing
-
Persistent bad breath or metallic taste
-
Receding gum lines that expose tooth roots
-
Loose or shifting teeth
-
Changes in bite alignment
Visual Changes:
-
Gums that appear bright red or purplish
-
Shiny or glossy gum surfaces
-
White or yellow pus between teeth and gums
-
Dark spaces appearing between teeth
Functional Problems:
-
Pain while chewing
-
Increased tooth sensitivity
-
Difficulty fitting partial dentures properly
Many people dismiss bleeding gums as normal, especially during brushing or flossing. However, healthy gums should never bleed during routine oral care. This bleeding signals inflammation and infection that requires attention.
How Gum Disease Progresses from Mild to Severe
Gum disease follows a predictable progression pattern, moving through distinct stages that increase in severity and complexity. Understanding this progression helps explain why early intervention proves so critical.
Stage 1: Gingivitis
The mildest form begins when bacterial plaque accumulates along the gumline. Gums become inflamed, red, and prone to bleeding. At this stage, the infection affects only the gum tissue itself, leaving the underlying bone and connective tissues undamaged. Complete reversal remains possible with improved oral hygiene and professional cleaning.
Stage 2: Early Periodontitis
Bacteria begin attacking the fibers and bone that support teeth. Small pockets form between teeth and gums, providing deeper spaces for bacteria to colonize. Gums start pulling away from teeth, and some irreversible damage occurs to the supporting structures.
Stage 3: Moderate Periodontitis
Bacterial infection reaches deeper levels, destroying more connective tissue and bone. Pockets between teeth and gums deepen significantly, often measuring 4-5 millimeters. Teeth may begin shifting or becoming loose as their support systems weaken.
Stage 4: Advanced Periodontitis
The final stage involves severe destruction of tissues and bone supporting teeth. Deep pockets form, often exceeding 6 millimeters in depth. Teeth become noticeably loose, may shift position, and often require extraction. The infection can spread to other areas of the mouth and body.
The Serious Health Consequences of Untreated Gum Disease
Research reveals that gum disease extends far beyond oral health concerns, creating pathways for bacteria to enter the bloodstream and affect multiple body systems. The chronic inflammation associated with gum disease triggers systemic responses that compromise overall health.
Cardiovascular Complications:
Studies demonstrate strong correlations between gum disease and heart disease. Bacteria from infected gums can enter blood vessels, contributing to arterial inflammation and increasing risks of heart attacks and strokes. People with severe gum disease show nearly twice the risk of developing coronary artery disease.
Diabetes Interactions:
Gum disease and diabetes create a dangerous cycle of mutual aggravation. Diabetics face higher risks of developing severe gum infections, while gum disease makes blood sugar control more difficult. The chronic inflammation from gum disease can worsen insulin resistance.
Respiratory Health:
Bacteria from the mouth can travel to the lungs, potentially causing or worsening respiratory conditions like pneumonia, chronic obstructive pulmonary disease (COPD), and other lung infections. This risk increases significantly in elderly populations and those with compromised immune systems.
Pregnancy Complications:
Pregnant women with gum disease face increased risks of premature birth, low birth weight babies, and pregnancy-related complications. Hormonal changes during pregnancy can worsen existing gum conditions, creating additional health risks for both mother and child.
Immune System Impact:
Chronic gum inflammation places constant stress on the immune system, potentially reducing its ability to fight other infections and diseases. This ongoing inflammatory burden can contribute to various autoimmune conditions and general health decline.
The financial implications also prove significant, as treating advanced gum disease and its related health complications costs substantially more than preventive care and early intervention.
Root Causes That Lead to Gum Disease Development
Poor Oral Hygiene Habits That Damage Your Gums
The foundation of gum disease lies in inadequate cleaning routines that allow harmful bacteria to flourish in the mouth. Brushing teeth less than twice daily creates an environment where plaque accumulates rapidly along the gum line, leading to inflammation and irritation. Many people rush through their oral care routine, spending less than the recommended two minutes brushing, which fails to remove bacteria effectively from all surfaces.
Skipping flossing represents one of the most damaging habits for gum health. Food particles and bacteria settle between teeth where toothbrush bristles cannot reach. Without daily flossing, these areas become breeding grounds for harmful microorganisms that produce toxins, causing gums to become swollen, tender, and prone to bleeding.
Using an old toothbrush with frayed bristles reduces cleaning effectiveness significantly. Dental professionals recommend replacing toothbrushes every three to four months, as worn bristles cannot properly disturb bacterial colonies. Additionally, aggressive brushing with hard bristles can damage delicate gum tissue, creating small wounds that bacteria can exploit.
Neglecting regular dental cleanings allows tartar buildup to harden below the gum line. Professional cleanings remove this stubborn deposit that home care cannot eliminate. Without these appointments, bacterial colonies establish deeper pockets around teeth roots, accelerating gum disease progression.
Lifestyle Factors That Increase Your Risk
Tobacco use stands as one of the most significant risk factors for developing gum disease. Smoking and chewing tobacco reduce blood flow to gum tissues, impairing the immune system’s ability to fight bacterial infections. Nicotine also masks early warning signs like bleeding gums, allowing the condition to advance unnoticed until more severe damage occurs.
Chronic stress weakens the body’s natural defense mechanisms, making it harder to combat bacterial infections in the mouth. High stress levels increase cortisol production, which suppresses immune function and reduces the body’s ability to heal damaged gum tissue. People under constant stress often neglect oral care routines, compounding the problem.
Poor dietary choices contribute significantly to gum disease development. Frequent consumption of sugary and processed foods feeds harmful bacteria in the mouth, creating acidic conditions that irritate gums. A diet lacking essential nutrients like vitamin C, calcium, and antioxidants fails to provide the building blocks necessary for healthy gum tissue maintenance and repair.
Excessive alcohol consumption creates a dry mouth environment by reducing saliva production. Saliva plays a crucial role in washing away bacteria and neutralizing acids. Without adequate saliva, bacterial colonies multiply more easily, increasing the likelihood of gum inflammation and infection.
Medical Conditions That Make You More Vulnerable
Diabetes creates a two-way relationship with gum disease, where each condition worsens the other. High blood sugar levels provide an abundant food source for oral bacteria, while gum infections can make blood sugar control more difficult. Diabetic patients experience slower healing times and increased inflammation, making their gums more susceptible to bacterial invasion and tissue damage.
Hormonal fluctuations during pregnancy, menstruation, and menopause significantly affect gum health. Increased hormone levels make gum tissue more sensitive to bacterial toxins, leading to swelling, tenderness, and bleeding. Pregnant women face particular risks, as pregnancy gingivitis can progress rapidly without proper care.
Autoimmune disorders like rheumatoid arthritis and lupus compromise the body’s ability to fight infections, including those affecting the gums. These conditions often require medications that further suppress immune function, creating additional vulnerability to bacterial overgrowth in the mouth.
Certain medications produce dry mouth as a side effect, reducing the protective benefits of saliva. Blood pressure medications, antidepressants, antihistamines, and pain relievers commonly cause this condition. Without adequate saliva production, bacteria multiply more freely, increasing the risk of gum disease development and progression.
Proven Daily Habits to Keep Your Gums Healthy
Master the Right Brushing Technique for Gum Protection
Effective brushing goes beyond simply moving a toothbrush around the mouth. The angle and pressure applied during brushing directly impact gum health and disease prevention. Position the toothbrush at a 45-degree angle toward the gum line, allowing the bristles to reach into the crevice where teeth meet gums. This technique helps remove bacteria and plaque buildup in areas where gum disease typically begins.
Gentle, circular motions work more effectively than aggressive back-and-forth scrubbing. Excessive pressure damages delicate gum tissue and can lead to recession over time. Spend at least two minutes brushing, dedicating equal attention to all areas of the mouth. Pay special attention to the gum line, as this area harbors the most harmful bacteria.
Replace toothbrushes every three to four months or when bristles begin to fray. Worn bristles lose their effectiveness and may harbor bacteria that contribute to gum inflammation.
Flossing Secrets That Actually Remove Harmful Bacteria
Daily flossing removes plaque and bacteria from spaces between teeth that brushes cannot reach. These interdental areas become breeding grounds for the bacteria responsible for gum disease when left uncleaned. Proper flossing technique involves wrapping approximately 18 inches of floss around the middle fingers, leaving about two inches of working floss.
Guide the floss gently between teeth using a rubbing motion, avoiding snapping or forcing the floss into place. Once the floss reaches the gum line, curve it into a C-shape against one tooth and slide it into the space between the gum and tooth. Use clean sections of floss for each tooth to avoid spreading bacteria throughout the mouth.
Water flossers serve as effective alternatives for people who struggle with traditional string floss. These devices use pressurized water to remove debris and bacteria from between teeth and below the gum line.
Choose the Best Oral Care Products for Gum Health
Selecting appropriate oral care products significantly impacts gum disease prevention efforts. Toothpastes containing fluoride strengthen tooth enamel and help fight cavity-causing bacteria that contribute to gum problems. Antimicrobial toothpastes specifically formulated for gum health contain ingredients like stannous fluoride or triclosan that target harmful bacteria.
Soft-bristled toothbrushes protect sensitive gum tissue while effectively removing plaque. Electric toothbrushes often provide superior plaque removal compared to manual brushes, making them valuable tools for gum disease prevention. Look for models with pressure sensors that alert users when brushing too hard.
Therapeutic mouthwashes containing antimicrobial ingredients provide additional protection against gum disease-causing bacteria. Products with the American Dental Association seal of acceptance have undergone rigorous testing for safety and effectiveness.
| Product Type | Key Features | Benefits for Gum Health |
|---|---|---|
| Antimicrobial Toothpaste | Contains stannous fluoride or triclosan | Targets harmful bacteria, reduces inflammation |
| Electric Toothbrush | Pressure sensor, timer | Superior plaque removal, prevents over-brushing |
| Therapeutic Mouthwash | ADA-approved antimicrobial agents | Reaches areas that brushing and flossing miss |
Create a Winning Daily Oral Care Routine
Establishing a consistent daily routine maximizes gum disease prevention efforts. Morning oral care should begin with flossing to loosen debris and bacteria, followed by thorough brushing and antimicrobial mouthwash. This sequence ensures maximum effectiveness of each step.
Evening routines hold particular importance since bacteria multiply rapidly during sleep when saliva production decreases. Repeat the flossing, brushing, and rinsing sequence before bed to remove the day’s accumulation of plaque and food particles.
Timing matters as much as technique. Wait at least 30 minutes after eating before brushing to allow saliva to neutralize acids produced by bacteria. Drinking water throughout the day helps rinse away food particles and maintains optimal saliva production for natural gum protection.
Regular dental checkups complement daily care routines by identifying early signs of gum disease before symptoms become apparent. Professional cleanings remove hardened plaque deposits that daily brushing cannot eliminate.
Professional Treatments That Reverse Gum Damage
Regular Dental Cleanings That Prevent Disease Progression
Professional dental cleanings serve as the cornerstone of gum disease prevention and early intervention. These routine appointments, typically scheduled every six months, go far beyond what daily brushing and flossing can achieve. Dental hygienists use specialized instruments to remove hardened plaque (tartar) that accumulates along the gum line and between teeth, areas that standard home care often misses.
During these sessions, the hygienist meticulously scales the teeth to eliminate bacterial buildup and polishes the surfaces to create a smooth environment that discourages future plaque formation. This process also includes thorough gum pocket measurements, allowing the dental team to monitor any changes in gum health over time. Regular cleanings catch the earliest signs of gum disease before symptoms become noticeable, making treatment more straightforward and less invasive.
For patients with a history of gum disease or those at higher risk, dentists may recommend more frequent cleanings every three to four months. This accelerated schedule helps maintain the progress made through previous treatments and prevents the condition from advancing to more severe stages.
Deep Cleaning Procedures That Restore Gum Health
When gum disease progresses beyond the earliest stages, standard cleanings become insufficient, and deep cleaning procedures become necessary. Scaling and root planing, commonly known as deep cleaning, represents the gold standard non-surgical treatment for moderate gum disease.
The scaling portion involves removing plaque and tartar from below the gum line, reaching into the pockets that form between the gums and teeth. Root planing follows, smoothing the tooth roots to eliminate bacterial toxins and create an environment where the gums can reattach to the teeth properly. This two-step process typically requires local anesthesia for patient comfort and may be completed over multiple appointments depending on the extent of the condition.
Advanced cases may benefit from additional procedures such as:
-
Laser therapy: Uses focused light energy to remove infected tissue and bacteria
-
Antibiotic treatments: Apply antimicrobial agents directly into gum pockets
-
Surgical interventions: Includes flap surgery or gum grafts for severe tissue damage
These procedures effectively halt disease progression and often reverse early to moderate gum damage when combined with improved home care.
When to Seek Immediate Professional Help
Recognizing the warning signs that require urgent dental attention can prevent irreversible damage to the gums and supporting bone structure. Bleeding gums during brushing or flossing, while common, should never be ignored as “normal.” Persistent bad breath that doesn’t improve with oral hygiene, swollen or tender gums, and loose teeth all signal the need for prompt professional evaluation.
Gum recession that exposes tooth roots creates sensitivity and increases infection risk, requiring immediate assessment. Pus discharge from the gums indicates active infection that may spread without proper treatment. Pain when chewing or changes in bite alignment suggest that gum disease has potentially affected the bone supporting the teeth.
Patients with certain medical conditions face elevated risks and should maintain closer contact with their dental team. Diabetes, heart disease, and pregnancy all create circumstances where gum infections can have serious systemic consequences. Individuals taking medications that cause dry mouth or those undergoing cancer treatments also need more frequent monitoring and intervention.
Emergencies include severe gum pain, facial swelling, fever accompanied by oral symptoms, or trauma to the mouth. These conditions require same-day dental care to prevent complications and preserve oral health.
Lifestyle Changes That Strengthen Your Gum Defense
Nutrition Strategies That Support Healthy Gums
The foods consumed daily play a crucial role in maintaining strong, healthy gums and preventing the progression of gum disease. Vitamin C stands as a powerhouse nutrient for gum health, supporting collagen production and tissue repair. Citrus fruits, berries, leafy greens, and bell peppers provide abundant vitamin C to strengthen gum tissue and boost the immune system’s ability to fight bacterial infections.
Omega-3 fatty acids found in salmon, sardines, walnuts, and flaxseeds offer anti-inflammatory properties that reduce gum inflammation and bleeding. These healthy fats help the body manage the inflammatory response that characterizes gum disease, creating an environment where healthy tissue can thrive.
Calcium and vitamin D work together to maintain strong teeth and supporting structures. Dairy products, fortified plant milks, and leafy greens supply calcium, while vitamin D enhances absorption and utilization. This combination helps maintain the bone structure that supports teeth and gums.
Antioxidant-rich foods combat the oxidative stress that contributes to gum disease progression. Green tea contains catechins that inhibit bacterial growth, while colorful vegetables and fruits provide various antioxidants that protect gum tissue from damage.
Limiting sugar intake prevents harmful bacteria from feeding and multiplying in the mouth. Processed foods, sugary drinks, and refined carbohydrates create an acidic environment that promotes bacterial growth and weakens gum tissue.
Break Harmful Habits That Destroy Gum Tissue
Tobacco use represents the most significant modifiable risk factor for gum disease development and progression. Smoking and chewing tobacco reduce blood flow to the gums, impair healing, and create an environment where harmful bacteria thrive. The chemicals in tobacco products weaken the immune system’s response to bacterial infections, making it nearly impossible for gums to heal naturally.
Teeth grinding and clenching, known as bruxism, place excessive pressure on gum tissue and can cause recession. This habit often occurs during sleep, making awareness and intervention challenging. Night guards and stress reduction techniques help protect gums from the damaging effects of grinding forces.
Nail biting introduces harmful bacteria from fingers into the mouth while potentially damaging gum tissue. This habit can cause small tears in the gums that become entry points for infection-causing bacteria.
Using teeth as tools to open packages, crack nuts, or hold objects places unnatural stress on gums and teeth. These activities can cause immediate trauma to gum tissue and create long-term problems with gum attachment.
An aggressive brushing technique damages delicate gum tissue and can cause recession over time. Using a soft-bristled toothbrush with gentle, circular motions protects gums while effectively removing plaque and bacteria.
Stress Management for Better Oral Health
Chronic stress significantly impacts gum health by suppressing immune function and increasing inflammation throughout the body, including the gums. High stress levels reduce the body’s ability to fight off bacterial infections, making gum disease more likely to develop and progress rapidly.
Stress often leads to poor oral hygiene habits as daily routines become disrupted. People under stress may skip brushing, forget to floss, or rely on quick fixes rather than thorough cleaning. This neglect allows plaque and bacteria to accumulate, creating ideal conditions for gum disease.
Cortisol, the primary stress hormone, increases inflammation in gum tissue and interferes with healing processes. Elevated cortisol levels also affect sleep quality, which further compromises immune function and the body’s ability to repair damaged tissue.
Regular exercise serves as a powerful stress reducer while improving circulation to the gum tissue. Physical activity helps manage cortisol levels and promotes better sleep, both of which support gum health and overall immune function.
Meditation and deep breathing exercises activate the body’s relaxation response, reducing stress hormones and inflammation. Even brief daily practice can lower stress levels and support better oral health outcomes.
Adequate sleep allows the body to repair and regenerate tissue, including gum tissue damaged by bacterial infection. Poor sleep quality weakens the immune response and makes gum disease more difficult to control, creating a cycle where stress impacts sleep, which affects gum health.
Conclusion
Gum disease affects millions of people worldwide, yet many cases remain preventable through proper oral care and healthy lifestyle choices. The journey from understanding the warning signs to implementing daily protective habits creates a solid foundation for maintaining optimal gum health. Regular brushing, flossing, and professional cleanings work together with smart dietary decisions and stress management to keep harmful bacteria at bay.
Taking action early makes all the difference when it comes to gum health. Professional treatments can effectively reverse damage when caught in time, but prevention remains the most powerful tool available. Start by evaluating current oral care routines and consider scheduling a dental checkup to assess gum health. Small changes made today can prevent serious complications down the road and contribute to better overall health for years to come.